Article Text
Abstract
Purpose: To report the technique of amniotic membrane transplantation dressing during the acute phase of Stevens-Johnson syndrome.
Methods: Interventional case report. We report the clinical presentation, surgical technique and clinical outcome of a patient with acute Stevens-Johnson syndrome and progressive tarsal conjunctival epithelial loss.
Results: A 10-year-old girl presented with extensive corneal, bulbar and tarsal conjunctival epithelial loss and severe ocular pain during the acute phase of Stevens-Johnson syndrome. Fornix cleaning and daily rodding was not tolerated, and there was no response to medical drug therapy. Emergency amniotic membrane transplant surgery was performed in both eyes. The conjunctival epithelium recovered completely and the ocular surface remained moist. There was almost complete resolution of ocular pain in the immediate postoperative period. There were no surgical complications and no signs of ocular cicatrisation after 6 months.
Conclusions: In the acute phase of severe Stevens-Johnson syndrome, conservative measures of daily fornix cleaning and rodding may not be practical. AMT dressing may be successfully used to reduce ocular inflammation, promote epithelialisation and prevent ocular cicatrisation.

To view the full report and accompanying video please go to: http://bjo.bmj.com/cgi/content/full/91/11/1536/DC1
All videos from the BJO video report collection are available from:
Statistics from Altmetric.com
Supplementary materials
Video Report
Technique of Amniotic Membrane Transplant Dressing in the Management of Acute Stevens-Johnson SyndromeE
Mahiul MK Muqit(1), Roger B Ellingham(1), Claire Daniel(2)1 Cornea and Anterior Segment Service, York Hospital NHS Trust, Wigginton Road, York, YO31 8HE, UK
2 Cornea and External Diseases Service, Moorfields Eye Hospital NHS Foundation Trust, 162 City Road, London, EC1V 2PD, UKCorrespondence: Dr Mahiul MK Muqit
Email: mmmk3{at}aol.com York Hospital NHS Trust, Wigginton Road, York, YO31 8HE, United Kingdom. Tel: 01904631313. Fax: 01904726343.Date of acceptance: 30th August 2007
Technique of amniotic membrane transplantation: Povidine iodine cleaning is followed by division of conjunctival adhesions and removal of conjunctival epithelial debris. Single sheet AMT is fixed to upper lid margin (6/0 dexon), and superior fornix bolster sutures placed below the upper brow (3/0 prolene). The AMT is sutured to the lower lid margin, and bolster sutures insert through the inferior fornix, at the infraorbital margin. At one week, the redundant amniotic membrane is excised from within the ocular sac, and the membrane has become adherent to the tarsal conjunctiva and lid margins. View Video: Fast connectionView Video: Dial up connection
Note: This video is best viewed in Quicktime
Introduction
Stevens-Johnson syndrome (SJS) is a rare and severe cutaneous reaction that may occur in children or adults. SJS is characterised by epidermal detachment that is preceded by immune-mediated keratinocyte apoptosis. Given the importance of immune mechanisms in SJS, amniotic membrane transplantation (AMT) is accepted as a potential treatment.1-3 We present a case of severe ocular SJS where conservative measures were not practical due to ocular pain, and we report our experience with AMT surgery during the acute phase.
Case Report
A 10-year-old girl presented to the paediatric service with a seven-day history of a viral illness, pyrexia, widespread blistering rash, and non-purulent conjunctivitis. Physical examination revealed an acutely ill child. Blanching, erythematous macules were scattered over her trunk and upper extremities, and confluent across the face. Mucous membrane examination showed swelling and fissuring of the lips, and superficial erosions of the tongue, soft palate, and pharynx. Ocular examination demonstrated a best-corrected Snellen visual acuity (BCSVA) of 6/9 O.D and 6/18 O.S. The eyelid margins were swollen and hyperaemic with bilateral conjunctival and left-sided central corneal epithelial loss.
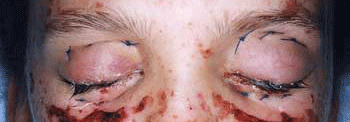
A diagnosis of drug-induced SJS was made. Management included a three-day course of intravenous methylprednisolone, hourly prednisolone 1% eyedrops, fusidic acid ointment twice-daily, and dexamethasone 0.1% ointment at night to both eyes. After 48 hours, the ocular picture had deteriorated and there was severe ocular pain. Almost 90% of the tarsal and bulbar conjunctiva had sloughed off with adhesions developing across the globe (Fig 1a,b). There was a large left-sided corneal epithelial defect with poor epithelialisation, and the BCSVA was reduced to 6/12 in both eyes. An emergency bilateral AMT dressing was proposed to control the ocular surface inflammation and prevent subconjunctival cicatrisation. Human AMT was obtained urgently from the Tissue Services in London, and surgery was performed on day 3 after presentation.



Figure 1 Pre-operative photos: after 48 hours, the ocular picture had deteriorated despite topical and systemic treatment. The conjunctiva was sloughing off with adhesions developing across the globe right eye (A) and left eye (B). Post-operative day 1: the superior and inferior fornix reformations sutures are visible (C) Surgical Technique
The technique is described for the left eye initially. In the operating room, povidine iodine irrigation of the conjunctival sac, eyelids, and eyelashes was performed. Loose, sloughed ocular tissue was removed. The conjunctival adhesions and symblepharon were divided, and the conjunctival epithelial debris was removed. The size of the membrane coverage was estimated across the whole ocular surface. A single sheet of human amniotic membrane was placed across the upper lid tarsus, and fixed to the upper lid margin with three double-ended 6/0 dexon grey line mattress sutures. The upper eyelid was double-everted with a Desmarres retractor to allow greater access to the superior fornix. The upper eyelid bolster sutures consisted of 3/0 prolene. The needle was passed from the amniotic membrane surface, through the superior fornix, through the full thickness of the upper lid and exited through the upper lid skin below the upper brow. Three suture knots were tied to anchor the membrane in the superior fornix. A grey line traction suture was inserted to assist in evertion of the upper eyelid. The free border of the amniotic membrane was laid across the lower tarsus and sutured to the lid margin with full-thickness bites. Inferior fornix reformation sutures included a triplet of 3/0 prolene sutures. The right eye underwent the same AMT surgical procedure at the same operative visit. The fellow ocular surface was dressed with two sheets of AMT joined at the lower limbus. Prophylactic topical and systemic antibiotic and steroid cover was continued.
On waking, the patient experienced immediate relief of her ocular discomfort (Fig1c). At one week postoperatively, the ocular inflammation settled and the corneal epithelium had healed completely. The AMT was trimmed within the ocular sac, and the membrane had become incorporated into the tarsal conjunctiva (Fig2) with no signs of symblepharon. BCSVA was 6/9 in both eyes. The patient was discharged from hospital one month after surgery. At eight weeks, the subjective refraction was plano O.D. and plano +0.25 x175 O.S, with BCSVA of 6/6 O.D. and 6/9 O.S. There was slight central corneal haze in the left eye, and faint scarring of the upper eyelid palpebral conjunctiva and trichiasis. All topical and systemic therapy was discontinued after two months. Distidiatic and trichiatic lashes were treated with electrolysis after 10 weeks. After six months, BCSVA was 6/5, and both eyes remained comfortable, moist with no signs of inflammation (fig 3). The patient has a good cosmetic appearance despite a slight asymmetric ptosis. There were no signs of limbal stem cell deficiency postoperatively.
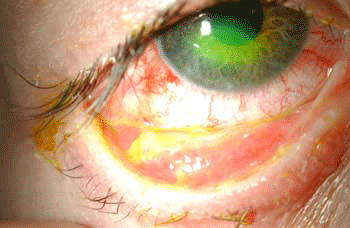


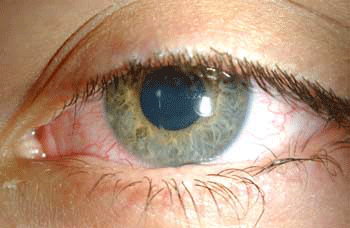
Figure 2 At one week, the amniotic membrane appears incorporated into the tarsal conjunctiva, right (A) and left (B) Figure 3 The ocular appearance after 6 months. Visual acuity: was 6/5 in both eyes. The ocular surface has remained non-inflamed and moist, with slight central corneal haze in the left eye (B) and lower lid lash misdirection. Discussion
Human amniotic membrane forms the innermost layer of the placenta, and consists of a single epithelial layer, avascular stroma and thick basement membrane.3 It has been used effectively for ocular surface reconstruction2. The AMT facilitates healing and regeneration of epithelial cells, prolongs epithelial stem cell survival, and reduces inflammation and scarring3. Growth factors are produced by the amnion, and it contains both anti-angiogenic and anti-inflammatory proteins that suppress neutrophil and macrophage infiltration. The basement membrane of the amnion supports the growth of epithelial progenitor cells. It facilitates migration of epithelial cells, promotes epithelial differentiation, reinforces adhesion of basal epithelial cells, and prevents epithelial apoptosis.
In conclusion, we present a patient with SJS with potential sight-threatening ocular complications. During the acute phase conservative measures were not possible, and medical therapy failed to prevent progression of ocular inflammation and loss of the corneal and conjunctival epithelia. Emergency AMT surgery was successfully performed after 48 hours. The anti-adhesive, anti-inflammatory and bandaging properties of AMT are beneficial for preserving ocular surfaces, reducing scarring, and relieving pain. A multidisciplinary approach is required in young children, and good communication and supportive treatment can effectively minimise the distress of this devastating condition.
Acknowledgement
We would like to thank John K Dart, Director of the Cornea and External Diseases Service, Moorfields Eye Hospital NHS Foundation Trust, London, UK, for his advice on the surgical technique used in this case.
Presented at the Royal College of Ophthalmologists Annual Congress 2007 and the British Association of Tissue Banking Annual Scientific Meeting 2007Conflict of Interest Statement
No conflicting relationship exists for any author, and there is no financial interest in any of the products mentioned in the article
References
- Puangsricharern V, Tseng SCG. Cytologic evidence of corneal diseases with limbal stem cell deficiency. Ophthalmology 1995;102:1476-85.
- Saw VP, Minassian D, Dart JK et al. Amniotic membrane transplantation for ocular disease: a review of the first 233 cases from the UK user group. Br J Ophthalmol 2007;91(8):1042-7.
- Dua HS, Gomes JA, King AJ et al. The amniotic membrane in ophthalmology. Surv Ophthalmol 2004;49(1):51-77.
Files in this Data Supplement:


