Abstract
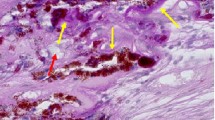
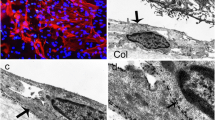
Eighteen patients with age-related macular degeneration developed subfoveal membranes that were surgically removed and submitted for histopathological examination. Immunohistochemical techniques were performed, using a panel of monoclonal antibodies recognizing retinal pigment epithelial (RPE) cells, myofibroblasts, pericytes, endothelial cells, glial cells, smooth muscle cells and various types of macrophages. The PC10 antibody to proliferating cell nuclear antigen (PCNA) was applied as a marker of proliferating cells. The specimens displayed a core of neovascular stroma surrounded by a rim of more fibrous tissue. All specimens contained abundant RPE cells that in some cases appeared to envelop part of the membrane. Most cases had basal laminar deposits and thickened basement membrane material adjacent to the RPE cells suggestive of parts of Bruch's membrane. Often this Bruchlike membrane appeared at the surgical margin, forming a surgical cleavage plane. Chronic inflammatory cells were abundant, but polymorphonuclear leukocytes were notably absent. Nearly all specimens contained myofibroblasts and various types of macrophages. The presence of myofibroblasts suggests subretinal membrane contraction, which may induce new breaks and other pathology in RPE layer and Bruch's membrane.
Similar content being viewed by others
References
Das A, Puklin JE, Frank RN, Zhang NL (1992) Ultrastructural immunocytochemistry of subretinal neovascular membranes in age-related macular degeneration. Ophthalmology 99:1368–1376
Doussis IA, Gatter KC, Mason DY (1993) CD68 reactivity in nonmacrophage derived tumours in cytological specimen. J Clin Pathol 46:334–336
Gabbiani G, Ryan GB, Majno G (1971) Presence of modified fibroblasts in granulation tissue and their possible role in wound contraction. Experientia 27:549–550
Green WR, Key SN III (1977) Senile macular degeneration: a histopathologic study. Trans Am Ophthalmol Soc 75:180–254
Green WR, McDonell PJ, Yeo JH (1985) Pathologic features of senile macular degeneration. Ophthalmology 92:615–627
Grossniklaus HE, Martinez JA, Brown VB, Lambert HM, Sternberg P Jr, Capone A Jr, Aaberg TM, Lopez PF (1992) Immunohistochemical and histochemical properties of surgically excised subretinal neovascular membranes in age-related macular degeneration. Am J Ophthalmol 114:464–472
Hasegawa T, Hirose T, Kudo E, Abe JI, Hizawa K (1990) Cytoskeletal characteristics of myofibroblasts in benign and reactive fibroblastic lesions. Virchows Archiv A Pathol Anat Histopathol 416:375–382
Hiscott P, Morino I, Alexander R, Grierson I, Gregor Z (1989) Cellular components of subretinal membranes in proliferative vitreoretinopathy. Eye 3:606–610
Landberg G, Roos G (1991) Antibodies to proliferating cell nuclear antigen as S-phase probes in flow cytometric cell cycle analysis. Cancer Res 51:4570–4574
Lopez PF, Grossniklaus HE, Lambert M, Aaberg TM, Capone A Jr, Sternberg P Jr, L'Hernault N (1991) Pathologic features of surgically excised subretinal neovascular membranes in age-related macular degeneration. Am J Ophthalmol 112:647–656
Lopez PF, Lambert M, Grossniklaus HE, Sternberg P (1993) Well-defined subfoveal choroidal neovascular membranes in age-related macular degeneration. Ophthalmology 100:415–422
Majno G, Gabbiani G, Hirschel BJ, Ryan GB, Statkov PR (1971) Contraction of granulation tissue in vitro: similarity to smooth muscle. Science 173:548–550
Sarks SH (1973) New vessel formation beneath the retinal pigment epithelium in senile eyes. Br J Ophthalmol 57:951–965
Smiddy WE, Maguire AM, Green WR, Michels RG, Cruz Z de la, Enger C, Jaeger M, Rice TA (1989) Idiopathic epiretinal membranes. Ultrastructural characteristics and clinicopathological correlation. Ophthalmology 96:811–821
Author information
Authors and Affiliations
Additional information
This paper was presented in part at the 1993 annual meeting of ARVO, Sarasota, Florida
Rights and permissions
About this article
Cite this article
Seregard, S., Algvere, P.V. & Berglin, L. Immunohistochemical characterization of surgically removed subfoveal fibrovascular membranes. Graefe's Arch Clin Exp Ophthalmol 232, 325–329 (1994). https://doi.org/10.1007/BF00175983
Received:
Revised:
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/BF00175983