Abstract
Aims/hypothesis
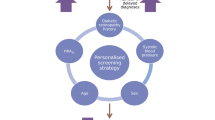
Our study aimed to validate a model to determine a personalised screening frequency for diabetic retinopathy.
Methods
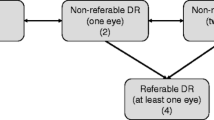
A model calculating a personalised screening interval for monitoring retinopathy based on patients’ risk profile was validated using the data of 3,319 type 2 diabetic patients in the Diabetes Care System West-Friesland, the Netherlands. Two-field fundus photographs were graded according to the EURODIAB coding system. Sight-threatening retinopathy (STR) was considered to be grades 3–5. Validity of the model was assessed using calibration and discrimination measures. We compared model-based time of screening with time of STR diagnosis and calculated the differences in the number of fundus photographs using the model compared with those in annual or biennial screening.
Results
During a mean of 53 months of follow-up, 76 patients (2.3%) developed STR. Using the model, the mean screening interval was 31 months, leading to a reduced screening frequency of 61% compared with annual screening and 23% compared with biennial screening. STR incidence occurred after a mean of 26 months after the model-based time of screening in 67 patients (88.2%). In nine patients (11.8%), STR had developed before the model-based time of screening. The discriminatory ability of the model was good (C-statistic 0.83; 95% CI 0.74, 0.92). Calibration showed that the model overestimated STR risk.
Conclusions/interpretation
A large reduction in retinopathy screening was achieved using the model in this population of patients with a very low incidence of retinopathy. Considering the number of potentially missed cases of STR, there is room for improvement in the model. Use of the model for personalised screening may eventually help to reduce healthcare use and costs of diabetes care.

Similar content being viewed by others
Abbreviations
- DCS:
-
Diabetes Care System West-Friesland
- STR:
-
Sight-threatening retinopathy
References
Ding J, Wong TY (2012) Current epidemiology of diabetic retinopathy and diabetic macular edema. Curr Diab Rep 12:346–354
Chalk D, Pitt M, Vaidya B, Stein K (2012) Can the retinal screening interval be safely increased to 2 years for type 2 diabetic patients without retinopathy? Diabetes Care 35:1663–1668
Olafsdottir E, Stefansson E (2007) Biennial eye screening in patients with diabetes without retinopathy: 10-year experience. Br J Ophthalmol 91:1599–1601
Rodbard HW, Blonde L, Braithwaite SS et al (2007) American Association of Clinical Endocrinologists medical guidelines for clinical practice for the management of diabetes mellitus. Endocr Pract 13(Suppl 1):1–68
Scanlon PH (2008) The English national screening programme for sight-threatening diabetic retinopathy. J Med Screen 15:1–4
Cheung N, Mitchell P, Wong TY (2010) Diabetic retinopathy. Lancet 376:124–136
Mehlsen J, Erlandsen M, Poulsen PL, Bek T (2011) Identification of independent risk factors for the development of diabetic retinopathy requiring treatment. Acta Ophthalmol 89:515–521
Stratton IM, Kohner EM, Aldington SJ et al (2001) UKPDS 50: risk factors for incidence and progression of retinopathy in Type II diabetes over 6 years from diagnosis. Diabetologia 44:156–163
Zavrelova H, Hoekstra T, Alssema M et al (2011) Progression and regression: distinct developmental patterns of diabetic retinopathy in patients with type 2 diabetes treated in the Diabetes Care System West-Friesland, the Netherlands. Diabetes Care 34:867–872
Agardh E, Tababat-Khani P (2011) Adopting 3-year screening intervals for sight-threatening retinal vascular lesions in type 2 diabetic subjects without retinopathy. Diabetes Care 34:1318–1319
Kohner EM, Stratton IM, Aldington SJ, Holman RR, Matthews DR (2001) Relationship between the severity of retinopathy and progression to photocoagulation in patients with Type 2 diabetes mellitus in the UKPDS (UKPDS 52). Diabet Med 18:178–184
Looker HC, Nyangoma SO, Cromie DT et al (2013) Predicted impact of extending the screening interval for diabetic retinopathy: the Scottish Diabetic Retinopathy Screening programme. Diabetologia 56:1716–1725
Porta M, Maurino M, Severini S et al (2013) Clinical characteristics influence screening intervals for diabetic retinopathy. Diabetologia 56:2147–2152
Stratton IM, Aldington SJ, Taylor DJ, Adler AI, Scanlon PH (2013) A simple risk stratification for time to development of sight-threatening diabetic retinopathy. Diabetes Care 36:580–585
Vijan S, Hofer TP, Hayward RA (2000) Cost–utility analysis of screening intervals for diabetic retinopathy in patients with type 2 diabetes mellitus. JAMA 283:889–896
Younis N, Broadbent DM, Vora JP, Harding SP (2003) Incidence of sight-threatening retinopathy in patients with type 2 diabetes in the Liverpool Diabetic Eye Study: a cohort study. Lancet 361:195–200
Aspelund T, Thornorisdottir O, Olafsdottir E et al (2011) Individual risk assessment and information technology to optimise screening frequency for diabetic retinopathy. Diabetologia 54:2525–2532
Welschen LM, van Oppen P, Dekker JM, Bouter LM, Stalman WA, Nijpels G (2007) The effectiveness of adding cognitive behavioural therapy aimed at changing lifestyle to managed diabetes care for patients with type 2 diabetes: design of a randomised controlled trial. BMC Public Health 7:74
Expert Committee on the Diagnosis and Classification of Diabetes Mellitus (2003) Report of the expert committee on the diagnosis and classification of diabetes mellitus. Diabetes Care 26(Suppl 1):S5–S20
Aldington SJ, Kohner EM, Meuer S, Klein R, Sjolie AK (1995) Methodology for retinal photography and assessment of diabetic retinopathy: the EURODIAB IDDM complications study. Diabetologia 38:437–444
Crowson CS, Atkinson EJ, Therneau TM (2013) Assessing calibration of prognostic risk scores. Stat Methods Med Res. doi:10.1177/0962280213497434
Harrell FE Jr, Lee KL, Mark DB (1996) Multivariable prognostic models: issues in developing models, evaluating assumptions and adequacy, and measuring and reducing errors. Stat Med 15:361–387
Ruamviboonsuk P, Teerasuwanajak K, Tiensuwan M, Yuttitham K (2006) Interobserver agreement in the interpretation of single-field digital fundus images for diabetic retinopathy screening. Ophthalmology 113:826–832
Healy R, Sallam A, Jones V et al (2013) Agreement between photographic screening and hospital biomicroscopy grading of diabetic retinopathy and maculopathy. Eur J Ophthalmol. doi:10.5301/ejo.5000404
Acknowledgements
We gratefully acknowledge M. S. A. Suttorp-Shulten (Department of Ophthalmology, OLVG, Amsterdam, the Netherlands) for grading of the fundus photographs.
Funding
This study was funded by ZonMw, the Netherlands organisation for health research.
Duality of interest
The authors declare that there is no duality of interest associated with this manuscript.
Contribution statement
AAWAvdH was involved in the conception and design of the study, analysis and interpretation of the data and drafting of the manuscript. IW was involved in the analysis and interpretation of the data and drafting of the manuscript. EvtR, TA, SHL, PE, BCPP, ACM, JEEK, JMD and GN were involved in the interpretation of the data and revision of the manuscript. GN was involved in the conception of the study, interpretation of the data and revision of the manuscript. All authors approved the final version of the manuscript. AAWAvdH and IW are the guarantors of this work, had full access to the data in the study and take responsibility for the integrity of the data and the accuracy of the data analysis.
Author information
Authors and Affiliations
Corresponding author
Additional information
A. A. W. A. van der Heijden and I. Walraven contributed equally to this study.
Electronic supplementary material
Below is the link to the electronic supplementary material.
ESM Methods
(PDF 73 kb)
Rights and permissions
About this article
Cite this article
van der Heijden, A.A.W.A., Walraven, I., van ’t Riet, E. et al. Validation of a model to estimate personalised screening frequency to monitor diabetic retinopathy. Diabetologia 57, 1332–1338 (2014). https://doi.org/10.1007/s00125-014-3246-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00125-014-3246-4