Abstract
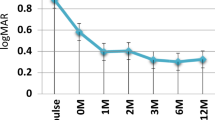
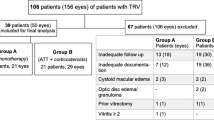
This study was undertaken to assess the efficacy of a standard regime of high-dose systemic oral corticosteroids in the management of retinal vasculitis. The study was performed because the single most common reason for referral to our specialist clinic is the apparent failure of patients to respond to a course of systemic steroids, which in most cases appeared to be due to an inadequate initial dose. A retrospective study of 29 patients (30 treatment episodes) with sight-threatening retinal vasculitis managed initially with high-dose systemic steroids was evaluated 1 year after treatment. Patients included in the study all started treatment with ≥ 1 mg/kg prednisolone and remained on a high steroid dose (≥40 mg prednisolone) for at least 5 weeks. No patient was on any other immunosuppressive agent at the start of the study. Therapeutic success for this regime, as judged by improvement in visual acuity, was 60%, improving to 77% with addition of other immunosuppressive agents. Eight patients required additional immunosuppressives. Although documented side-effects of steroids were common (50% of cases managed on steroids alone), in only 5 patients were they therapeutically important. Twelve of the 22 patients managed on high-dose steroids alone were off treatment at 12 months. There was no correlation at any stage between visual acuity, activity index or relapses and the final visual outcome at 12 months. Seven cases had a poor visual outcome and the causes for this included relapse in the twelfth month of follow-up, persistent cystoid macular oedema and lens opacity. These results suggest that high-dose oral steroids should be tried in the initial management of such patients before contemplating other more complicated regimes or accepting a poor visual outcome.
Similar content being viewed by others
Article PDF
References
Gordon DM . Hydrocortisone in ophthalmology. Am J Ophthalmol 1954; 37: 533–8.
Gordon DM . Prednisone and prednisolone in ocular disease. Am J Ophthalmol 1956; 41: 593–600.
Forrester JV . Uveitis: pathogenesis. Lancet 1991; 338: 1498–501.
Hemady R, Tauber J, Foster CS . Immunosuppressive drugs in immune and inflammatory ocular disease. Surv Ophthalmol 1991; 35: 369–85.
Lightman S . Use of steroids and immunosuppressive drugs in the management of posterior uveitis. Eye 1991; 5: 294–8.
Benezra D, Cohen E . Treatment and visual prognosis in Behçet's disease. Br J Ophthalmol 1986; 70: 589–92.
Nussenblatt RB, Palestine AG, Chan CC, Stevens G, Mel low SD, Green SB . Randomized double-masked study of cyclosporine compared to prednisolone in the treatment of endogenous uveitis. Am J Ophthalmol 1991; 112: 138–46.
Dumonde DC, Kasp-Grochowska E, Graham E, Sanders MD, Faure JP, de Kozak Y, van Tuyen V . Anti-retinal auto-immunity and circulating immune complexes in patients with retinal vasculitis. Lancet 1982; 2: 787–92.
Stanford MR, Graham E, Kasp E, Sanders MD, Dumonde DC . A longitudinal study of clinical and immunological findings in 52 patients with relapsing retinal vasculitis. Br J Ophthalmol 1988; 72: 442–7.
Santamaria J . Steroidal agents: their systemic and ocular complications. Ocular Inflammation Ther 1983; 1: 19–26.
Fauci AS . Haynes BF, Katz P . The spectrum of vasculitis: clinical, pathological, immunologic and therapeutic considerations. Ann Intern Med 1978; 89: 660–76.
Nussenblatt RB, Palestine AG . Cyclosporin: immunology, pharmacology and therapeutic uses. Surv Ophthalmol 1986; 31: 159–69.
Schein PS, Winokur SH . Immunosuppressive and cytotoxic chemotherapy: long term complications. Ann Intern Med 1975; 82: 84–95.
Goodman LS, Gilman AG . The Pharmacological basis of therapeutics. Oxford: Pergamon Press, 1990:1270–1.
Bennett WM, Pulliam JP . Cyclosporine nephrotoxicity. Ann Intern Med 1983; 99: 851–4.
Towler HMA, Cliffe AM, Whiting PH, Forrester JV . Low dose cyclosporine A therapy in chronic posterior uveitis. Eye 1989; 3: 282–7.
Towler HMA, Whiting PH, Forrester JV . Combination low dose cyclosporin A and steroid therapy in chronic intraocular inflammation. Eye 1990; 4: 514–20.
Palestine AG, Nussenblatt RB, Chan CC . Side effect of systemic cyclosporine in patients not undergoing transplantation. Am J Med 1984; 77: 652–6.
Myers BD, Ross J, Newton L, Ruetscher J, Perlroth M . Cyclosporine associated chronic nephropathy. N Engl J Med 1984; 311: 699–705.
Palestine AG, Austin HA, Barlow JE, Antonovych TT, Sabins SG, Preuss HG, Nussenblatt RB . Renal histopathological alterations in patients treated with cyclosporine for uveitis. N Engl J Med 1986; 314: 1293–8.
Svenson K, Bohmen SO, Hällgren R . Renal interstitial fibrosis and vascular changes: occurrence in patients with autoimmune diseases treated with cyclosporine. Arch Intern Med 1986; 146: 2007–10.
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Howe, L., Stanford, M., Edelsten, C. et al. The efficacy of systemic corticosteroids in sight-threatening retinal vasculitis. Eye 8, 443–447 (1994). https://doi.org/10.1038/eye.1994.105
Issue Date:
DOI: https://doi.org/10.1038/eye.1994.105
Keywords
This article is cited by
-
T lymphocyte insensitivity to corticosteroids in chronic obstructive pulmonary disease
Respiratory Research (2012)
-
Mycophenolate mofetil therapy in uveitis: analysis of eight cases in a tertiary ophthalmic care centre in India
International Ophthalmology (2009)
-
Visual outcome of patients with central eales disease
Annals of Ophthalmology (2001)
-
Efficacy of oral methotrexate pulsed therapy in eales disease
Annals of Ophthalmology (2000)
-
The role of azathioprine in the management of retinal vasculitis
Eye (1998)